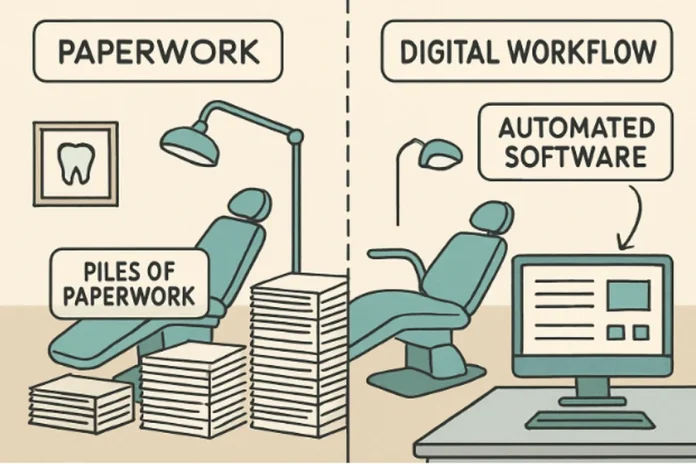
Dental insurance claims have long been a source of frustration for both dental practices and their patients. The arduous process—full of paperwork, administrative overhead, and frequent reimbursement delays—can drain resources and increase stress across the board. Today, industry leaders are turning to automation and artificial intelligence (AI) to modernize claims workflows, making them faster, more reliable, and less prone to costly mistakes. In fact, most dental claims support systems now leverage some form of digital automation for efficiency.
Automation isn’t just a lofty goal—it’s increasingly becoming the norm for practices seeking to maintain high levels of service and financial predictability. By reducing manual work, dental offices speed up billing cycles and empower staff to focus more on patient care. When practices streamline claims management, they can help minimize errors, improve transparency, and shorten payment wait times.
The Challenges of Traditional Claims Processing
Traditional dental insurance claims processes can be complex and inefficient. Manual data entry, reliance on paper documentation, and back-and-forth communications with insurance companies make these workflows vulnerable to errors and unnecessary delays. Even minor inaccuracies in patient data or coding can result in a claim denial, disrupting cash flow and potentially affecting the patient’s ability to continue care.
For small practices, the challenge is even greater—limited staffing means a single overlooked detail can create outsized problems downstream. Extended wait times for approvals and reimbursements can leave dental offices in limbo, forcing them to rely on outdated methods that fail to keep pace with modern expectations.
Many practices face challenges when deciphering constantly evolving insurance policies and coding requirements. Without centralized updates or clear communication channels, offices spend countless hours just keeping up, which can directly hamper productivity and morale.
Automation: Enhancing Efficiency
Automation is transforming how dental support staff handle claims. With automated tools, practices can streamline coverage verification, expedite claims submissions, and reduce duplicate data entry. Reports estimate that automation could save the dental industry as much as $2.6 billion every year by reducing redundancies and human errors. Automation platforms also help manage follow-ups on outstanding claims, reducing administrative burden and helping practices keep their focus on delivering care rather than chasing paperwork.
The best automated systems offer seamless integration with practice management software, allowing staff to check patient coverage, update records, and submit claims all in one place.
AI: Transforming Claims Management
AI is revolutionizing the dental claims world by providing real-time analysis and auditing of claims data. AI-powered engines review billing codes and claims submissions for accuracy, spotting inconsistencies and potential issues before they reach insurers. Furthermore, AI can predict the likelihood of claim approvals using historical data, providing dental teams with actionable insights for future submissions. Some AI tools even recommend the optimal time to submit claims, further accelerating reimbursements.
Real-Time Eligibility Verification
One of the most impactful advances in claims processing is the adoption of real-time eligibility verification. By instantly checking a patient’s insurance status at the point of scheduling or service, offices can confirm coverage, estimate out-of-pocket costs, and reduce the risk of claim denials. Automated eligibility verification systems provide a reliable way to ensure claims are filed correctly the first time, reducing wait times and eliminating surprises for both staff and patients.
Leading digital verification tools quickly pull up patient benefits information, coverage limits, and other essential details, all without phone calls or manual checks. This tool is especially valuable during busy clinic hours when administrative efficiency is crucial.
Improving Patient Experience
Patients want clarity about what their insurance will cover and how much they will owe. Studies show that 78% of dental patients prioritize transparency around insurance coverage, while 93% expect proactive payment reminders to help manage their care. Practices that use automated claims and real-time verification systems can provide patients with faster, more precise cost estimates, reducing uncertainty and building trust. Effective automation also reduces the likelihood that patients will be surprised by unexpected bills after treatment.
Improved communication and reduced paperwork make the care journey smoother, freeing up staff time to focus on clinical service and patient engagement rather than bureaucratic tasks. As a result, practices see higher patient satisfaction, fewer complaints, and better retention rates.
Future Trends in Claims Processing
The path forward in dental insurance claims management lies in deeper integration of AI with other digital technologies. Machine learning algorithms will soon handle coding and billing end-to-end—from interpreting clinical notes to preparing claims for different payers. Meanwhile, blockchain technology is emerging as a way to provide a secure, transparent ledger of claims activities, promising to reduce fraud further and simplify audits. By providing all stakeholders—practices, insurers, and patients—with a shared, tamper-proof record, blockchain could become a cornerstone in building trust and improving efficiency in dental payments, as outlined in recent research published by the American Dental Association.
As these technologies evolve, dental practices can expect more intuitive claims software, faster reimbursements, and an even greater focus on the patient experience.
Conclusion
The integration of automation and AI into dental insurance claims is transforming how administrative processes are managed across the industry. By optimizing workflows, minimizing mistakes, and enhancing patient experiences, dental practices can strengthen both their financial performance and quality of service. Adopting these advanced technologies allows clinics to remain competitive, ensuring efficient operations and satisfied patients well into the future. As these innovations advance, they will continue to refine billing procedures and boost the precision of claims handling. In turn, automation and AI enable dental teams to dedicate more time to delivering exceptional patient care rather than managing paperwork.